Cartilage, a remarkable tissue found throughout the animal kingdom, often goes unnoticed until we experience its discomfort. While we commonly associate our skeletal system with rigid bones, it's the resilient, smooth, and often hidden presence of cartilage that enables much of our body's flexibility, cushioning, and effortless movement. What makes this connective tissue truly unique, and perhaps most intriguing, is its ability to perform these vital functions without the direct support of a blood supply or nervous system. This avascular and aneural nature poses significant challenges, particularly when it comes to nutrition and repair. So, how does this vital, insensate tissue sustain itself, and what hope does it have for healing when damaged?
The Unique Nature of Cartilage: Avascular and Aneural
At its core, cartilage is a specialized form of connective tissue, designed for resilience and elasticity. Unlike bone, it's not hard and rigid; yet, it's considerably stiffer than muscle or tendon. This semi-transparent, non-porous material is primarily composed of specialized cells called chondrocytes, which are embedded within a vast extracellular matrix (ECM). This matrix, rich in water, collagen fibers, and proteoglycans, gives cartilage its characteristic firmness, flexibility, and rubbery consistency.
The most defining characteristic of cartilage, particularly when discussing its nutrient supply and repair capabilities, is its avascular and aneural status. To say that cartilage is avascular means it contains no blood vessels. This immediately sets it apart from nearly every other tissue in the body, which relies on a direct blood supply for oxygen and nutrient delivery, as well as waste removal. Similarly, being aneural means it lacks nerves, making it insensitive to pain or other stimuli. While this insensitivity can be a double-edged sword – preventing immediate pain signals when damage occurs – it also means the tissue has no direct way to communicate its needs or status.
A Closer Look at Cartilage Composition and Function
The chondrocytes, though sparsely distributed, are the master builders of cartilage. They actively produce and maintain the complex extracellular matrix that surrounds them. This matrix is a dynamic blend of components:
- Collagen Fibers: Primarily Type II collagen, these provide tensile strength and structure.
- Proteoglycans: Large molecules like aggrecan, which attract and trap water, giving cartilage its turgor and ability to resist compression.
- Glycosaminoglycans (GAGs): Complex carbohydrates that are part of proteoglycans, further enhancing water retention.
- Elastin (in elastic cartilage): Provides additional flexibility, allowing the tissue to spring back into shape.
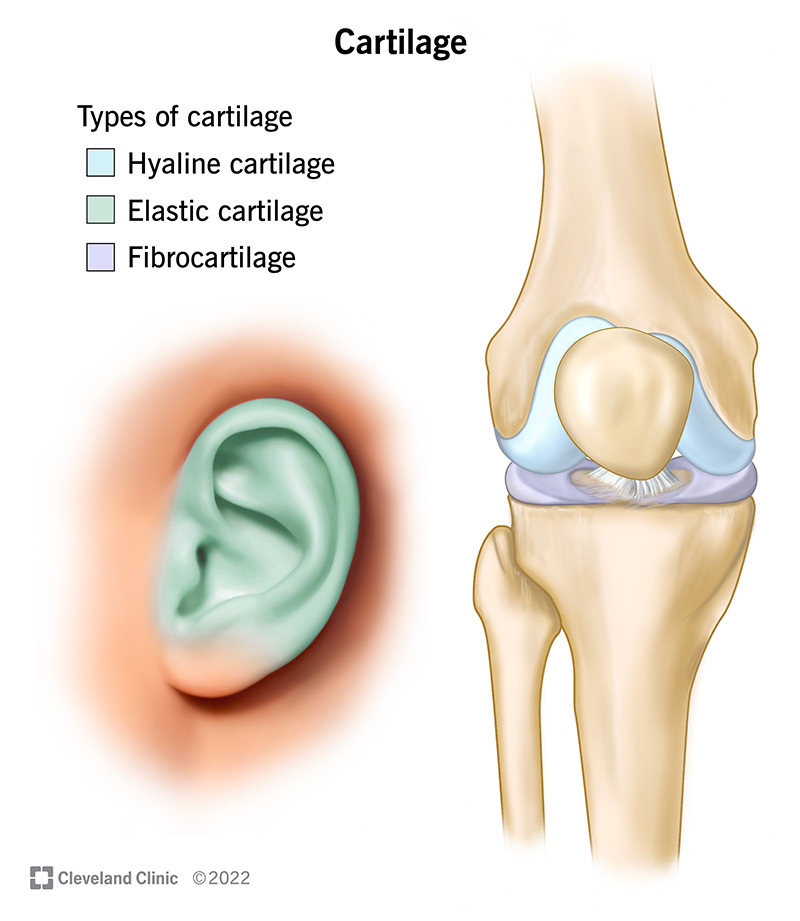
The specific proportions of these components classify cartilage into three main types: hyaline, elastic, and fibrocartilage, each suited for different functional demands across the body. From cushioning the ends of long bones in joints (articular cartilage) to providing structural support in the rib cage, nose, and trachea, Cartilage Explained: Function, Types, and Body Support details its critical roles. In essence, cartilage acts as a robust shock absorber, a smooth gliding surface, and a resilient structural framework.
The Ingenious Nutrient Delivery System for Avascular Tissue
Given its lack of blood vessels, the question of how cartilage obtains its vital nutrients becomes paramount. The answer lies in a clever, albeit slower, process: diffusion, significantly aided by mechanical forces.
Diffusion: The Lifeline for Chondrocytes
Diffusion is the passive movement of molecules from an area of higher concentration to an area of lower concentration. For chondrocytes nestled deep within the cartilage matrix, this is their primary mode of receiving oxygen, glucose, and other essential nutrients, as well as expelling metabolic waste products.
But diffusion needs a source. Where do these nutrients originate?
- Synovial Fluid: For articular cartilage, which covers the ends of bones within joints, the main source of nutrition is the synovial fluid. This viscous, egg-white-like fluid fills the joint cavity, lubricating the joint and acting as a nutrient-rich bath. Nutrients from the synovial fluid diffuse directly into the articular cartilage.
- Perichondrium: Most other cartilage types (like elastic cartilage in the ear or hyaline cartilage in the trachea) are typically enveloped by a tough, fibrous membrane called the perichondrium. This membrane is vascularized, meaning it *does* contain small blood vessels. Nutrients diffuse from these vessels within the perichondrium, across the membrane, and into the cartilage tissue itself.
The Crucial Role of Mechanical Loading and Fluid Flow
Diffusion alone would be too slow to sustain metabolically active chondrocytes, especially those deep within thicker cartilage. This is where mechanical forces come into play, essentially acting as a pump:
- Compression and Decompression: When articular cartilage in a joint is subjected to compression (e.g., during walking or standing), fluid within its matrix is squeezed out, carrying waste products. When the pressure is released (decompression), the cartilage acts like a sponge, drawing in fresh, nutrient-rich synovial fluid from the joint space. This "milking" action is vital for maintaining cartilage health.
- Flexion: Similarly, the flexion and extension of elastic cartilage (e.g., in the external ear) or the movement of structural cartilage also generate fluid flow, facilitating the diffusion process.
This interdependence between mechanical loading and nutrient delivery highlights why movement and moderate exercise are so critical for cartilage health. Immobility can starve cartilage of its essential supplies, leading to degeneration.
How Different Cartilage Types Get Nourished
While diffusion is universal, the precise nutrient source can vary slightly among Hyaline, Elastic & Fibrocartilage: Understanding Each Type:
- Hyaline Cartilage: In joints, it relies on synovial fluid. In other areas (like the trachea or nose), it relies on the perichondrium.
- Elastic Cartilage: Typically covered by a perichondrium, from which it receives nutrients.
- Fibrocartilage: Often found in high-stress areas like intervertebral discs and the menisci of the knee. Interestingly, some fibrocartilage, such as the outer regions of the meniscus, has a partial blood supply. This slight vascularization offers a marginally better capacity for nutrient delivery and, consequently, repair compared to completely avascular cartilage.
Understanding Cartilage Repair: A Slow and Complex Process
The avascular nature of cartilage, while efficient for nutrient delivery with movement, presents significant challenges when it comes to repair. Compared to most other connective tissues, cartilage has an incredibly slow turnover of its extracellular matrix and is notorious for repairing at a very slow rate, if at all.
The Challenge of Self-Repair
When cartilage is damaged, particularly articular cartilage, the body's intrinsic repair mechanisms are severely limited. Here's why:
- No Direct Blood Supply: The absence of blood vessels means no direct route for inflammatory cells, growth factors, or repair cells to reach the site of injury. Blood clots, which are the first step in the healing cascade for most tissues, cannot form directly within avascular cartilage.
- Chondrocyte Limitations: Mature chondrocytes are terminally differentiated, meaning they have a limited capacity to divide and proliferate. They are also relatively immobile within their lacunae, making it difficult for them to migrate to the site of injury and initiate repair.
- Avascularity Limits Response: Without nerves, the cartilage itself doesn't "feel" the injury in the traditional sense, and without blood vessels, it can't mount a typical inflammatory response, which is crucial for initiating repair in other tissues.
The Nature of Cartilage Repair
When natural repair does occur, it's often a suboptimal process:
- Limited Intrinsic Repair: Chondrocytes adjacent to the injury might attempt to synthesize new matrix components, but this is usually insufficient to repair significant defects.
- Fibrocartilage Formation: If the injury extends into the underlying bone (subchondral bone), which is vascular, blood can enter the defect. This can lead to the formation of a fibrous clot. However, the cells that migrate into this clot often differentiate into fibroblasts, which then produce fibrocartilage. While this fills the defect, fibrocartilage is mechanically inferior to the original hyaline cartilage, being less resilient and prone to premature degeneration, especially in weight-bearing joints.
- Poor Integration: Newly formed repair tissue often struggles to integrate seamlessly with the surrounding healthy cartilage, creating weak points that can fail under stress.
Due to these inherent limitations, significant cartilage injuries rarely heal completely or restore the original tissue's function, often leading to chronic pain, reduced mobility, and the progression of conditions like osteoarthritis.
Practical Tips for Supporting Cartilage Health and Repair
While cartilage's repair capacity is limited, proactive measures can significantly support its health and potentially slow down degeneration:
- Movement is Medicine: Regular, moderate physical activity is paramount. Low-impact exercises like swimming, cycling, and walking encourage the essential fluid flow through cartilage, delivering nutrients and removing waste. Avoid prolonged immobility.
- Balanced Nutrition: Provide your body with the building blocks for healthy cartilage. Focus on a diet rich in:
- Vitamin C: Crucial for collagen synthesis.
- Lean Proteins: To support overall tissue repair.
- Omega-3 Fatty Acids: May help reduce inflammation.
- Specific Supplements: Glucosamine and chondroitin sulfate are often used for joint health. While research on their efficacy varies, some individuals report benefit. Always consult a healthcare professional before starting any supplements.
- Maintain a Healthy Weight: Excess body weight significantly increases the load on articular cartilage, especially in weight-bearing joints like the knees and hips, accelerating wear and tear.
- Prevent Injuries: Use proper form during exercise, warm up adequately, and use protective gear when appropriate. Avoid repetitive high-impact activities if you have pre-existing cartilage concerns.
- Stay Hydrated: Water is a major component of cartilage matrix. Adequate hydration supports the turgor and resilience of the tissue.
Cartilage stands as a testament to the body's remarkable adaptive capabilities. Despite its avascular and aneural nature, it performs crucial roles in cushioning, support, and movement, relying on an ingenious system of diffusion and mechanical loading for its survival. While its limited capacity for self-repair underscores the importance of prevention and early intervention for injuries, understanding how this vital tissue functions empowers us to make lifestyle choices that support its longevity and contribute to overall joint health.